Why the Weeks After Ramadan Deserve Your Attention
For many residents across the UAE, Ramadan brings a profound shift in daily life. Eating and drinking patterns change entirely, sleep is reorganised around prayer and community, and the body adapts in ways both visible and invisible. Most people move through the month with remarkable resilience. But when the fast ends, and the rhythm of everyday life gradually resumes, certain health markers can shift in ways that are easy to overlook.

Weight, blood sugar, and blood pressure are three of the most telling indicators of how the body has responded to a month of significant metabolic change. For individuals who are generally healthy, a brief period of monitoring and recalibration is usually all that is needed. For those managing chronic conditions, the post-Ramadan period calls for a more deliberate and medically supported approach.
Understanding what to watch for, and knowing when to involve your family doctor, can make a meaningful difference to your health in the months ahead.
What Happens to the Body During and After Fasting
Ramadan fasting is not simply skipping meals. It involves extended daily periods without food or water, often paired with disrupted sleep and increased physical and social activity in the evenings. The body responds by drawing on stored energy, adjusting hormone levels, and modifying how it processes glucose and fat.
For many people, these adaptations produce measurable changes in blood sugar regulation, weight, and cardiovascular markers. Some of those changes are beneficial. Others require monitoring and, in some cases, medical review. The challenge is that these shifts do not always produce obvious symptoms. A person can feel perfectly well while their blood pressure has crept upward or their blood sugar has become less stable than it was before the fast began.
This is one of the reasons why post-Ramadan monitoring matters, not as a cause for alarm, but as an act of informed, preventive care.
Tracking Your Weight After Eid
Weight changes during Ramadan vary considerably from person to person. Some individuals lose weight through caloric restriction and dehydration. Others gain weight, particularly if iftar and suhoor meals were calorie-dense or if activity levels dropped significantly during the month. The celebratory meals of Eid itself can add another layer of change in a short period of time.
What is most important in the weeks following Eid is not the number on the scale in isolation, but the trend and the context. A few things worth noting:
- Sudden weight loss may reflect fluid changes rather than fat loss, and hydration needs to be restored gradually
- Gradual weight gain over Ramadan that continues after Eid may indicate a pattern worth discussing with a doctor
- Significant changes in appetite, persistent bloating, or unusual fatigue alongside weight changes may warrant a clinical review
- For individuals on structured weight management programmes, reconnecting with their care team after Eid is an important step
Weight is one of the most modifiable health markers, and it has direct implications for blood pressure, blood sugar, and cardiovascular risk. Monitoring it consistently, in the context of your broader health picture, gives your family doctor a far more useful picture than a single reading taken in isolation.
Blood Sugar: The Marker That Needs Closest Attention
For individuals with diabetes or prediabetes, blood sugar monitoring after Ramadan is not optional. It is essential. Medication regimens are frequently adjusted during Ramadan to accommodate the fasting schedule, and those adjustments need to be reviewed and often reversed once regular eating patterns resume. Continuing a Ramadan-modified medication plan into the weeks after Eid can lead to either inadequately controlled blood sugar or, in some cases, hypoglycaemia.
Even for individuals without a diagnosed condition, the post-Ramadan period is a valuable time to check fasting glucose levels. The combination of altered eating patterns, sleep disruption, and dietary changes during the month can unmask early glucose regulation issues that were previously subclinical.
Our chronic disease management service at Westminster Clinic is designed precisely for this kind of ongoing, personalised monitoring. Rather than treating each blood sugar reading as an isolated data point, our family physicians track patterns over time and adjust care plans in response to what they observe across weeks and months.
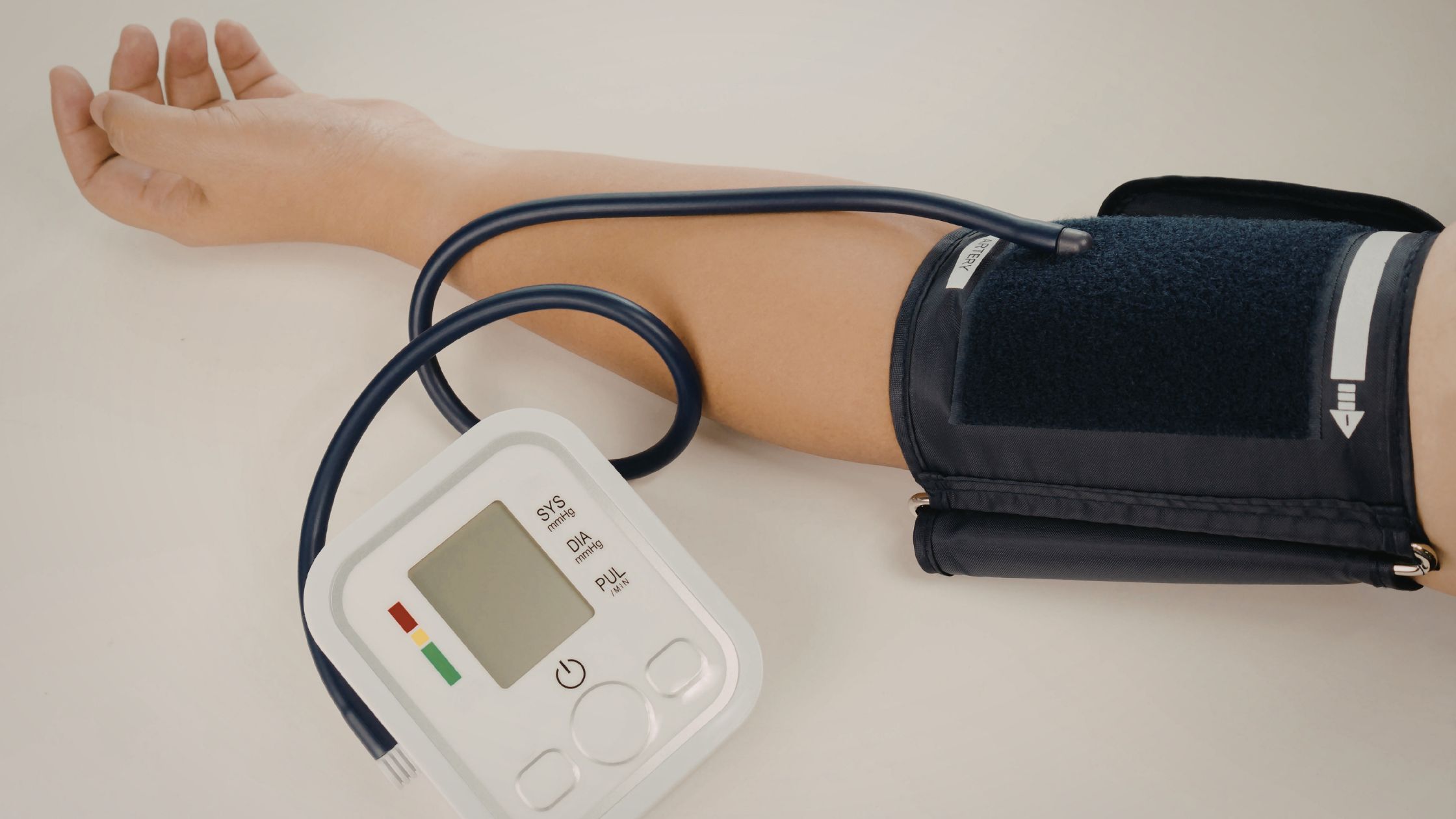
Blood Pressure: The Silent Marker
Hypertension earns its reputation as a silent condition because it rarely announces itself through noticeable symptoms. During Ramadan, blood pressure can fluctuate in both directions. Some individuals experience a modest reduction in blood pressure during fasting periods, which is generally positive. Others, particularly those who consume high-sodium foods at iftar or suhoor, or who experience significant sleep disruption, may see their blood pressure rise.
After Eid, the return to normal eating, combined with the lingering effects of a disrupted sleep cycle, can produce readings that differ meaningfully from a person’s usual baseline. For those already on antihypertensive medication, a post-Ramadan review of dosage and timing is often warranted. For those who have not had their blood pressure checked recently, this is an excellent moment to do so.
A general health checkup or annual wellness exam will typically include a blood pressure reading alongside other key markers, making it a practical and efficient way to get a clear picture of where you stand after the month.
The Case for Consistent, Ongoing Monitoring
One of the most common patterns in preventive medicine is this: people check their health markers when something feels wrong, and then stop checking once they feel better. This is understandable, but it misses the point of monitoring entirely.
Blood sugar, blood pressure, and weight are most informative when tracked consistently over time, with a doctor who knows your history. A single reading tells you very little. A trend tells you a great deal. Our family medicine services are structured around this principle of continuity, where your care does not begin and end with a single consultation, but builds over time into a genuinely personalised understanding of your health.
For patients managing multiple conditions simultaneously, our ongoing monitoring and medication adjustment service ensures that changes in one marker are considered in the context of the others, and that your treatment plan evolves as your health does.
After Ramadan Is the Right Time to Check In
There is a tendency to view the post-Ramadan period as simply a return to normal, as if the month can be set aside and life resumes unchanged. In reality, the body takes time to recalibrate, and for those with existing health conditions or risk factors, that recalibration deserves medical support.
You do not need to feel unwell to benefit from a check-in. A brief review of your key markers, a conversation about how your body responded to the fast, and a clear plan for the months ahead is exactly the kind of care that prevents problems from developing quietly in the background.
This is what family medicine, at its best, looks like: attentive, continuous, and built around knowing you well enough to notice when something has shifted.
Plan Your Post-Ramadan Health Review
Our experienced family physicians at Westminster Clinic in Dubai Healthcare City welcome patients who want to take a proactive approach to their health after Ramadan. Whether you are managing an existing chronic condition, monitoring risk factors, or simply want to know where your key health markers stand, we are here to support you with thorough, personalised care.
To find out more about how we support patients with long-term health monitoring, visit our family medicine services page, or schedule a consultation with our team at a time that works for you. Patients from across Dubai are warmly welcome, as are those travelling from Abu Dhabi or Al Ain.

